A historic meeting between chiropractic and Make America Healthy Again (MAHA) leadership took place on March 10th, 2026, in Washington, D.C., featuring representatives from chiropractic national organizations, professional associations and policy principals. The collective goal: advancing the role of chiropractic in improving the health of Americans. Meeting participants focused on long-standing issues that have affected the chiropractic profession for decades, including access to care, reimbursement parity, and ensuring DCs have an appropriate role in national health policy discussions.
| Digital ExclusiveAvocados to Guacamole Can Be Dangerous: Axis Fracture From Picking Avocados
In California, there are many avocado groves. The trees grow very tall - up to 30 feet. People still pick avocados by hand, and sometimes it can be dangerous work.
A patient fell while picking avocados. He was diagnosed with several fractured ribs and then sent home to recover. After being off of work for three months, he presents to the office with a complaint of constant headaches and neck pain. He has very limited range of motion in the cervical spine. Due to the marked limitation of motion and apparent discomfort, you decide not to conduct orthopedic tests without taking X-rays of the cervical spine first.
Can you just rely on the patient's X-ray report? Let's say you decide to just take a lateral and APOM X-ray just to make certain nothing has changed since the patient fell. That was a long way to fall if the history is correct.
The lateral view isn't very helpful, but the APOM demonstrates a slight depression of the lateral mass of C2 on one side compared to the opposite side. Other than that finding, nothing really appears to be significant. If you didn't have the history, would you have taken the X-rays? If you didn't have the history and the clinical findings, would you have noticed the difference in the lateral masses of C2? It's difficult to say. I'm not certain I would, but the patient had significant discomfort.



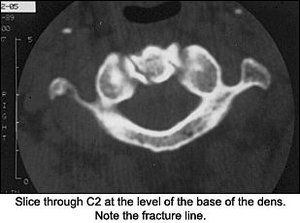


So, what would you do now with this information? Perform orthopedic tests, or would you do further imaging? I decided on more imaging because I'm into radiology. I really didn't want to do any orthopedic tests on the patient because having him run through simple range of motion of the cervical spine aggravated his symptoms, so I ordered a CT of the cervical spine. Upon review of the X-rays, we can now see that the APOM was telling us the answer we couldn't see clearly.
On the CT scan through the C1-2 vertebrae, note the fracture through the dens and the lateral mass of C2. (That was the depression we saw on the APOM of the lateral mass.) Should we look at the APOM view again?
This view above evaluates C1-C2, which cannot be visualized clearly on the lateral. The most important element to check is the alignment of the lateral masses of C1. The intervertebral space should be symmetric. The dens can also be evaluated for fracture in this view, but occasionally overlying shadows may give the false impression of a dens fracture (Mach effect). Correlate the findings with the lateral view of the cervical spine. The incidence of fractures to the axis is about 6 percent, and over 50 percent of those fractures involve some part of the dens.
I can't say I would have picked up this finding in a stack of films that I read over a day, especially since I rarely get any clinical information. Did they make guacamole out of the avocados that fell along with the patient? I can't answer that question, either.
Deborah Pate, DC, DACBR
San Diego, California
patedacbr@cox.net



