A historic meeting between chiropractic and Make America Healthy Again (MAHA) leadership took place on March 10th, 2026, in Washington, D.C., featuring representatives from chiropractic national organizations, professional associations and policy principals. The collective goal: advancing the role of chiropractic in improving the health of Americans. Meeting participants focused on long-standing issues that have affected the chiropractic profession for decades, including access to care, reimbursement parity, and ensuring DCs have an appropriate role in national health policy discussions.
| Digital ExclusiveIs It Safe to Adjust the Cervical Spine in the Presence of a Herniated Disc?
I am often asked by chiropractors, medical doctors and patients if manipulation of the cervical spine is safe in the presence of a cervical herniated nucleus pulposis (CHNP). I usually answer that in most circumstances it not only is safe, but it is often an essential aspect of treatment. I will clarify what this means and provide some of the evidence that supports this notion. I will also illustrate that in most of cases that require treatment, manipulation alone is not a sufficient approach, but that some form of rehabilitation is necessary.
Radiculopathy resulting from CHNP, while less common than its counterpart in the lumbar spine, is common enough that most chiropractors can expect to see at least several per year. Unlike in the lumbar spine, there is a wide variation in the natural history of this disorder. Many patients do quite well with very little or no treatment, while a few, particularly those patients that have a traumatically- induced CHNP, require extensive treatment and rehabilitation; others fall somewhere between these extremes.
Let us start by discussing the anatomy of CHNP. The anatomy of the cervical disc is different than the lumbar disc. The nucleus pulposis of the cervical disc is smaller than the lumbar disc.1 The nucleus of the cervical disc undergoes desiccation much sooner than the lumbar disc. That process begins during adolescence and usually results in complete conversion to fibrocartilage by age 40.2 One would think, then, that it is almost impossible for an adult to develop CHNP, but, obviously, clinical experience suggests otherwise. With aging, clefts develop in the cervical disc, which accompanies desiccation.1 This cleft development may help explain why adults can develop CHNP, even if there is a relative paucity of water in the nucleus.
(Note: Recent research3 suggests that there are even greater differences in the anatomy of the cervical disc compared to the lumbar, but further work is required to verify this.)
In addition to the presence of discal clefts, tears can develop in the annulus that can contribute to the formation of a channel through which the nucleus can migrate (See Figure 1).
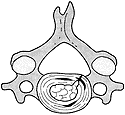
Disc derangement. From Murphy DR, ed. Conservative Management of Cervical Spine Syndromes. New York: McGraw-Hill, 1999. With permission.
If these channels extend to the periphery of the annulus, the nucleus has a path through which it can herniate and become exposed to the periradicular space (Figure 2). This can then cause irritation and/or compression of the nerve root, depending on whether there is actual physical pressure present or whether there is merely chemical irritation. If, at the same time, joint dysfunction is present at the same segment, the hypomobility that results may create a fluid stasis, which may then increase the intensity of chemical irritation to the nerve root. Joint dysfunction may also create pain on its own.
My experience is that joint dysfunction is often present at the level of CHNP. When joint dysfunction is present, the cases are more severe. The cases without joint dysfunction are far easier to manage, often needing very little or no treatment beyond monitoring neurologic status, providing anti-inflammatory and analgesic strategies in the acute stage, and assessment for cervical stability and the need for stabilization training in the subacute stage.
If there is joint dysfunction present at the level of HNP, should the patient be adjusted? With the treatment of choice for joint dysfunction being manipulation, the obvious answer is yes.
But what about the dangers of adjusting someone with a CHNP? There are some who consider the presence of HNP in the cervical spine an outright contraindication for manipulation.4 However, the vast majority of chiropractors (who perform the majority of manipulations in this country),5 consider this in the presence of CHNP to be safe and appropriate.6 While no large-scale studies have been conducted regarding the complication rate of manipulation in the presence of CHNP, several cases have been reported in the literature describing patients having been treated in this manner without aggravation of the condition, let alone serious complication.7-10 In one study,7 11 patients with CHNP were treated with an approach that included manipulation; nine of them were able to return to their previous occupations. No complications were reported. Certainly, as someone who has treated scores of patients with CHNP over the years, my experience with the relative safety of manipulation for this condition is consistent with that suggested by the literature.
There is very little information available in the literature on the mechanism of CHNP. Most of what is discussed is based on studies on the lumbar spine. While the types of strains which cause damage to the cervical disc may not be exactly the same as those that injure the lumbar disc, it is still believed that repetitive flexion combined with rotation and axial loading are most significant.11 While many types of cervical manipulation involve flexion and/or rotation, they certainly do not involve axial loading and are not applied repetitively over a long period of time.
Still, care needs to be taken when applying manipulation to a segment in which CHNP is present, as an acutely inflamed nerve root can be quite sensitive and it is easy to provoke pain. The maneuvers should be gentle (this applies to any manipulation) and the segment should be carefully taken to the barrier (the point at which tension first becomes palpable12) before thrust is applied. Extension should be avoided, as this increases IVF pressure.13 It is often helpful to apply long-axis traction while carrying out the manipulation, as this has been shown to decrease pressure in the disc.14
It is my opinion that cervical manipulation in the presence of CHNP should never be applied unless the practitioner is qualified.15 Chiropractors, by virtue of their knowledge, training and experience are in a unique position to be the ones to provide this treatment for patients suffering from radiculopathy related to CHNP. However, the complexity of this condition is such that merely knowing how to manipulate does not necessarily give one the ability to properly manage the case as a whole. Knowing when to apply rehabilitation procedures, such as cervical stabilization,16,17 over-the-door traction,15 medications, and what self-care strategies to employ are all vital items of information. Of equal importance is deciding when no treatment is necessary, if the practitioner is going to function as a physician rather than just a manipulative therapist.
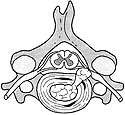
Disc herniation. From Murphy DR, ed. Conservative Management of Cervical Spine Syndromes. New York: McGraw-Hill, 1999. With permission.
Manipulation to the cervical spine in the presence of CHNP can be considered a safe and effective part of an overall management strategy for patients with radiculopathy. However, it must be carried out in a skilled and precise fashion and it must not be seen as the end point of care, but rather as one piece in the puzzle. The other pieces must include anti-inflammatory measures, self-care strategies and rehabilitation. It also must be recognized that many of these patients require very little treatment and will do well with a minimum of intervention.
References
- Eliot D. Functional anatomy of the cervical spine. Murphy DR, ed. Conservative Management of Cervical Spine Syndromes. New York: McGraw-Hill, 1999:3-23.
- Bland JH, Boushey DR. Anatomy and physiology of the cervical spine. Sem Arthritis Rheum 1990; 20:1-20.
- Mercer S, Bogduk N. The ligaments and annulus fibrosus of human adult cervical intervertebral discs. Spine 1999;24(7):619-626.
- Rogers C, Joshi A, Dreyfuss P. Cervical intrinsic disc pain and radiculopathy. Malanga GA, ed. Cervical Flexion-Extension/ Whiplash Injuries. Spine: State of the Art Reviews 1998; 12(2):323-356.
- Bigos S, Bowyer O, Braen G, et al. Acute Low Back Problems in Adults. Clinical Practice Guideline, Number 14. AHCPR Pub. No. 95-0642. Rockville, MD: Agency for Health Care Policy and Research, Public Health Service, US Department of Health and Human Services, December 1994.
- Croft AC. Appropriateness of cervical spine manipulation in disc herniation: a survey of practitioners. Chiro Tech 1994; 8(4):178-179.
- BenEliyahu DJ. Chiropractic management and manipulative therapy for MRI documented cervical disk herniation. J Manipulative Physiol Ther:1994:17(3):177-185.
- Brouillette DL, Gurske DT. Chiropractic treatment of cervical radiculopathy caused by a herniated cervical disc. J Manipulative Physiol Ther 1994:17(2):119-123.
- Pollard H, Tuchin P. Cervical radiculopathy: a case for ancillary therapies?. J Manipulative Physiol Ther. 1995; 18(4):244-249.
- Hughes BL. Management of cervical disk syndrome utilizing manipulation under anesthesia. J Manipulative Physiol Ther 1993; 16(3):174-18
- Gordon SJ, Yang KH, Mayer PJ, Mace AH, Kish VL, Radin EL. Mechanism of disc rupture: a preliminary report. Spine 1991;16(4):450-456.
- Lewit K. Management of muscular pain associated with articular dysfunction. Man Med 1991; 6(4):140-142.
- Farmer JC, Wisneski RJ. Cervical spine nerve root compression: an analysis of neuroforaminal pressures with varying head and arm positions. Spine 1994; 19(16):1850-1855.
- Yi-kai L, Qing-an Z, Shi-zhen Z. The effect of cervical traction combined with rotatory manipulation on cervical nucleus pulposus pressures. J Manipulative Physiol Ther 1998; 21(2):97-100.
- Murphy DR, Gruder MI, Murphy LB. Cervical radiculopathy and pseudoradicular syndromes. Murphy DR, ed. Conservative Management of Cervical Spine Syndromes. New York: McGraw-Hill, 1999:189-219.
- Murphy DR. Sensorimotor training and cervical stabilization. In: Murphy DR, ed. Conservative Management of Cervical Spine Syndromes. New York: McGraw-Hill, 1999:607-640
- Saal JS, Saal JA, Yurth E. Nonoperative management of cervical intervertebral disc with radiculopathy. Spine 1996; 21(16):1877-1883.
- Dillin W, Uppal GS. Analysis of medications used in the treatment of cervical disk degeneration. Orthop Clin North Am 1992; 23:421-433.



