A historic meeting between chiropractic and Make America Healthy Again (MAHA) leadership took place on March 10th, 2026, in Washington, D.C., featuring representatives from chiropractic national organizations, professional associations and policy principals. The collective goal: advancing the role of chiropractic in improving the health of Americans. Meeting participants focused on long-standing issues that have affected the chiropractic profession for decades, including access to care, reimbursement parity, and ensuring DCs have an appropriate role in national health policy discussions.
| Digital ExclusiveSensory-Motor Training, Part I
Sensory motor training is a valuable form of active care. It requires minimal cost to utilize in the clinical setting, and home-training balance equipment is also inexpensive ($25-$50). This form of therapy should form a basic component of the rehabilitation service alongside training aimed at strength, endurance, cardiovascular fitness and flexibility.
The propriosensory system helps the motor system to maintain equilibrium on a reflex, automatic basis. According to Winter, "Because 2/3 of our body mass is 2/3 of body height above the ground, we are an inherently unstable system, unless a control system is operating." (Winter 1995) In response to a sudden load, "the muscles will respond rapidly to stabilize the body, i.e., they will try to maintain balance and posture."(Wilder, et al.,1996).
Poor balance has been correlated with ataxia; low back pain; neck pain; cervicobrachial syndromes; ankle instability and sprain; and knee instability and osteoarthritis. Additionally, balance training has been shown to be successful in remedying many of these conditions. Balogun, et al., showed that balance board training could be a very efficient tool in rehabilitation because it actually produced greater lower extremity strength gains than did a series of isotonic exercises taking far longer (Balogun, et al., 1992). Sensory motor therapy with balance sandals has been shown to increase the speed of contraction of key hip stabilizers (Bullock-Saxton, et al., 1993, Janda, Va'vrova' 1996).
Brandt, et al., found that the elderly with ataxia can be treated successfully with balance training (Brandt 1981). Two weeks of training to significant improvement nine months later, without any home maintenance program. In another five-week balance program, only shorter-term results were achieved, suggesting for maintenance of results, training may need to continue (Seidler 1997). Two different trials of Tai Chi showed that a longer-term program improves balance abilities of older adults and that improvement persisted after training stopped (Wolf, et al., 1996, Wolfson, et al., 1996).
Balance in low-back-pain patients has been found to be impaired compared to asymptomatic subjects (Byl, Sinnot 1991, Alexander, et al., 1998, Luoto, et al., 1998, Mientjes, et al., 1999, Takala, et al., 1998). Balance has been shown to be disturbed in individuals with neck pain as well as cervicobrachial pain syndromes (Lewit 1988, Karlberg, et al., 1995, McPartland, et al., 1997).
Balance training can improve postural sway and single-leg standing balance in patients with functional ankle instability (Bernier, Perrin 1998, Rozzi, et al., 1999). Six weeks of balance training improved balance and stability in soccer players with functional instability (Tropp, et al., 1984a, Gauffin, et al., 1998). It also prevented future injuries in soccer players with ankle instability (Tropp, et al., 1985). A five-week wobble-board training program has been shown to improve movement discrimination for both ankles in elite rugby league players (Waddington, et al., 1999).

Figure 1: Single-leg- standing balance test |
It has been shown that individuals who underwent sensory-motor (SM) training improved their hamstring reaction time whereas those that underwent resistance training did not (Ihara, Nakayama 1986). Poor balance has been found in individuals with bilateral knee osteoarthritis more so than in an age-matched control group (Wegener, et al., 1997). Poor balance has also been identified in ACL-deficient knees (O'Connell, et al., 1998). In a prospective, controlled study of over 900 athletes, it has been shown that soccer players who undergo balance training can prevent ACL injuries (Carrafa 1996).
Evaluation
Balance can be assessed with the single-leg stance test (Janda 1996, Bohannon, et al., 1984), and can be quantified (Bohannon, et al., 1984). The patient may perform this by raising one foot without touching it to the support leg; begin with the eyes open, practicing once or twice on each side; then, with gaze fixed straight ahead, have the patient close his or her eyes and maintain balance up to 30 seconds. Failure occurs if the foot touches the leg on the support leg; hopping occurs; the foot touches the floor; or the arms touch something for support. The patient should be given two to four chances to reach peak performance.
Sensory-Motor Training
Sensory-motor (SM) training is easy to incorporate into a rehabilitation program. It basically involves training the patient in proper foot position, and then facilitating reflex balance responses. Modeling of the "short" foot, and rocker, wobble board and balance sandal training are the key "tools of the trade."
SM training begins with careful attention to formation of an actively shortened longitudinal arch of the foot without flexion of the toes (Bullock-Saxton, et al., 1993, Janda, Va'vrova' 1990;Janda, Va'vrova' 1996). This "short foot" is based on the work of Freeman, et al. (Freeman, et al., 1965 - see Figure 2). Freeman demonstrated that a short foot," position would increase proprioceptive outflow. Patients often have difficulty consciously producing the "short foot" and thus, a number of alternatives to formation of the "short foot" have been suggested. Turning the knees out without moving the feet is an easy "trick" that lifts the arch.. Lewit recommends gripping with the toes to activate the deep arch muscles (Lewit 1999). Exercises proceed from sitting to standing and from stable to labile surfaces. The "short foot" position is maintained throughout most of the exercises.
An excellent beginning balance exercise is simply to stand on one leg in a doorway for 30 seconds (see Figure 1). This can be progressed to performing with eyes closed. The patient should be encouraged to avoid reaching out, and if he or she can't last the full 30 seconds, the patient may do a few repetitions until 30 seconds are achieved cumulatively. This exercise should be performed twice a day.

|

|
In standing, various leaning movements are introduced and explored. A single step taken forward with a forward lean (i.e., lunge) and held emphasizes alignment, coordination and balance. The same is done with a single backward step with the torso aligned upright and the ischia over the heels. Lunges can be performed slowly six to twelve times, once per day.
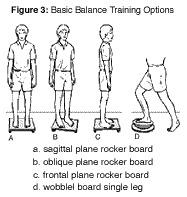
To further challenge reflexive righting movements, the subject is placed on a labile surface i.e., a rocker board - see Figure 3. The rocker board is unstable in one plane only. The patient stands on the board in various directions in order to control the plane of instability. Again, the exercises proceed from two-leg standing to single-leg standing, and unexpected pushes or other cervicovestibular or vestibular-ocular challenges are utilized to elicit an improved reflex response (Janda,Va'vrova 1990, Janda, Va'vrova' 1996). Balance board training should last between five and 30 minutes per day.
|

|
Janda has devised a unique pair of balance sandals (from OPTP) consisting of a rigid sole configured to support the longitudinal arch and metatarsal heads as in the "small foot" (Bullock-Saxton, et al., 1993, Janda, Va' vrova'1990; Janda, Va'vrova' 1996 - see Figure 4). On the bottom of the sole, a rigid hemisphere about the size of a tennis ball is fixed at the midway point. This essentially creates a pair of mini wobble boards to carefully walk upon. The goal is to walk very slowly, taking tiny steps initiated by lifting the knees up. The patient should practice stepping in place, while near a wall for support. Progressions include taking small steps forward, backwards, and sideways. At all times the "small foot" should be maintained, and the sandals platform should be kept as level as possible. In one study, after two weeks of prescribed exercise, the speed of contraction of the gluteus maximus and medius were increased by as much as 180-200 percent, and remained so as much as six weeks postexercise without further reinforcement (Bullock-Saxton, et al., 1993). The patient should attempt to practice with the balance sandals five minutes a session - three times a day.
A patient with decreased balance ability should be progressed through a balance training program which stays at a fairly challenging level so that it does not become boring. The office and home routines will often vary. In the office, "reflex pushing" and more advanced balance apparatus can be used. At home, once patients learn to perform the "small foot" or gripping exercise and can stand for 30 seconds on one leg with their eyes closed they are ready for a home tool such as the rocker board or balance sandals.
Conclusion
Balance is as important as strength or flexibility to overall physical fitness. Most injuries occur suddenly when an unexpected force is encountered, such as when an ankle is sprained by stepping off a curb an individual doesn't realize is there. This illustrates that balance is even more important than strength in injury prevention.
Balance training has been utilized for treating athletes with ankle sprains, children with vestibular (inner ear) problems, chronic knee injuries, elderly individuals with ataxia (frequent falls), and even lower back pain. Balance training has been shown to be more efficient than strength training and to result in very rapid training results. It is not arduous and can be fun for patients, resulting in relatively good compliance and motivation
References
- Bologun JA, Adesinasi CO, Marzouk DK 1992. The effects of a wobble board exercise training program on static balance performance and strength of lower extremity muscles. Physiother Can 44:23-30.
- Bernier JN. Perrin DH 1998. Effect of coordination training on proprioception of the functionally unstable ankle. J Orthop Sports Phys Ther 27:264-275.
- Bohannon RW, Larkin PA, Cook AC, Gear J, Singer J 1984. Decrease in timed balance test scores with aging. Physical Therapy 64;7:1067-1070.
- Brandt T, Krafczyk S, Malsbendend I 1981. Postural imbalance with head extension: improvement by training as a model for ataxia therapy. Ann NY Acad Sci 636-649.
- Bullock-Saxton JE, Janda V, Bullock MI 1993. Reflex activation of gluteal muscles in walking. Spine 18:6;704-708.
- Byl NN, Sinnot PL 1991. Variations in balance and body sway in middle aged adults: Subjects with healthy backs compared with subjects with low-back dysfunction. Spine 16:325-330.
- Carrafa A., Cerulli G, Projectti M, Aisa G, Rizzo A 1996. Prevention of anterior cruciate ligament injuries in soccer. A prospective controlled study of proprioceptive training. Knee Surg Sports Traumatol Arth 4(1):19-21.
- Freeman MAR, Dean MRE, Hanham IWF 1965. The etiology and prevention of functional instability of the foot. J Bone and Joint Surg (Br) 47B: 678-685.
- Gauffin H, Tropp H, Odenrick P 1988. Effect of ankle disk training on postural control in patients with functional instability of the ankle joint. Int J Sports Med 9:141-144.
- Ihara H, Nakayama A 1986. Dynamic joint control training for knee ligament injuries. Am J Sports Med 14(4);309-31.
- Janda V, Va' vrova' M 1996. Sensory motor stimulation. In Liebenson C (ed) Spinal Rehabilitation: A Manual of Active Care Procedures. Williams and Wilkins, Baltimore.
- Janda V, Va' vrova' M 1990. Sensory Motor Stimulation: A video. Presented by JE Bullock-Saxton. Brisbance, Australia, Body Control Systems.
- Karlberg M, Persson L, Magnusson M 1995. Reduced postural control in patients with chronic cervicobrachial pain syndrome. Gait and Posture 3:241-249.
- Lewit K 1988. Disturbed balance due to lesions of the cranio-cervical junction. J Orth Med 3:58-61.
- Lewit K 1999. Manipulative Therapy in Rehabilitation of the Motor System. 3rd edition. London: Butterworths.
- Luoto S, Aalto H, Taimela S, Hurri H, Pyykko I, Alaranta H 1998. One-footed and externally disturbed two-footed postural control in patients with chronic low back pain and healthy control subjects. Spine 23:2081-2090.
- McPartland JM, Brodeur RR, Hallgren RC 1997. Chronic neck pain, standing balance, and suboccipital muscle atrophy -a pilot study. J Manipulative Physiol Ther 20:24-29.
- Mientjes MIV, Frank JS 1999. Balance in chronic low back pain patients compared to healthy people under various conditions in upright standing. Clin Biomech 14:710-716.
- O'Connell M, George K, Stock D 1998. Postural sway and balance testing: a comparison of normal and anterior cruciate ligament deficient knees. Gait and Posture 8:136-142.
- Rozzi SL, Lephart SM, Sterner R, Kuligowski L 1999. Balance training for persons with functional unstable ankles. J Orthop Sports Phys Ther 29:478-486.
- Seidler R, Martin PE 1997. The effects of short-term balance training on the postural control of older adults. Gait and Posture 6:224-236.
- Takala EP, Korhonen I, Viikari-Juntura E 1998. Postural sway and stepping response among working population. Reproducibility, long-term stability, and associations with symptoms of the low back. Clin Biomec 12:429-437.
- Tropp H, Askling C 1984a. Effects of ankle disk training on muscular strength and postural control . Am J Sports Med 85:259-61.
- Tropp H, Ekstrand J, Gillquist J 1984b. Stabilometry in functional instability of the ankle and its value in predicting injury. Medicine and Science in Sports and Exercise 16:64-66.
- Tropp H, Ekstrand J, Gillquist J 1984c. Factors affecting stabilometry recordings of single limb stance. Am J of Sports Med 12:185-188.
- Tropp H, Askling C, Gillquist J 1995. Prevention of ankle sprains. Am J of Sports Med 4:259-262.
- Waddington G, Adams R, Jones A 1999. Wobble board (ankle disc) training effects on the discrimination of inversion movements. Australian J of Physio 45:95-101.
- Wegener L, Kisner C, Nichols D 1997. Static and dynamic balance responses in persons with bilateral knee osteoarthritis. J Orthop Sports Phys Ther 25:13-18.
- Wilder DG, Aleksiev AR, Magnusson ML, Poper MH, et al., 1996. Muscular response to sudden load. Spine 21 (22):2628-2639.
- Winter DA 1995. Human balance and posture control during standing and walking. Clin Biomech, 3(4)193-214.
- Wolf SL, Barnhart HX, Kutner NG, et al., 1996. Reducing frailty and falls in older persons: An investigation of Tai Chi and computerized balance training. JAGS 44:489-497.
- Wolfson L, Whipple R, Derbe C, et al., 1996. Balance and strength training in older adults: Intervention gains and Tai Chi maintenance. JAGS 44:498-506.
Craig Liebenson,DC
Los Angeles, California
cldc@flash.net



