The proposed merger of the National Board of Chiropractic Examiners and Federation of Chiropractic Licensing Boards was approved by NBCE delegates and FCLB members at their respective annual meetings, held jointly in Atlanta, Ga., this year. Per the new bylaws, the new entity takes the NBCE name, with FCLB continuing as a department within NBCE. The federation will continue to enjoy Board of Directors representation on what will be a single, expanded board.
| Digital ExclusiveHeel Pain: Fasciitis or Nerve Entrapment?
Have you ever treated a plantar fasciitis that did not respond? It might be a nerve entrapment. The symptoms between these two conditions often are strikingly similar. There might not be any paraethesiae on nerve compression, Tinel sign or even a loss of sensation in the area. Both may exhibit symptoms of heel pain upon arising, possibly lessening during the day, with localized pain at the medial process of the calcaneal tuberosity.
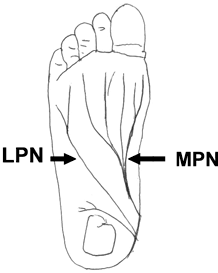
The tibial nerve runs posterior to the medial malleolus under the flexor retinaculum (Tarsal canal) and divides into the medial plantar nerve (MPN), the lateral plantar nerve (LPN) and the medial calcaneal branches. Compression at the tarsal canal (tarsal tunnel syndrome) could be responsible for heel pain. Half the time, the cause is idiopathic, but a synovial cyst, ganglion protruding from a tendon sheath, a lipoma, severe pronation, valgus hindfoot or severe ankle sprain might be the cause.1
Most patients with a tarsal tunnel complain of a burning, tingling or numb feeling on the plantar portion of the foot. Sometimes the pain is localized to one of the three terminal branches, emulating a plantar fasciitis. A possible differentiation from plantar fasciitis is that while in both diagnoses, the pain is aggravated by activity and relieved by rest, with entrapment, there might be relief by getting up, moving around and even massaging the foot. It is possible there might be fluid accumulation around the nerve during rest and during the first steps. The fluid pressure causes pain, but with walking, the venous pooling and intracompartmental pressures reduce. This might be a reason that pain of neural origin may decrease with walking. However, pain on walking also might decrease in plantar fasciitis.
With entrapment, pain also could occur with rest and in nonweight-bearing positions not common in fasciitis. Tapping the posterior tibial nerve first above the malleolus, and then distally to the terminal branches, might elicit tingling.
The entrapment site thought to be the most common cause of plantar heel pain is the first branch of the LPN. This nerve can get trapped where it passes at the sharp edge of the deep fascia of the abductor hallucis, just distal to the medial edge of the calcaneous, and especially when there is a calcaneal spur or even an association with a plantar fasciitis.2 Maximal tenderness should be over the nerve, although there might be tenderness over the heel and proximal plantar fascia.
Coppieters, et al., evaluated a modified straight-leg-raising test (SLRTIBIAL) that helps to differentiate plantar fasciitis from a neural problem.3 The clinician first dorsiflexes and everts the ankle, and then flexes the hip with a SLR. The addition of hip flexion further increased the mechanical forces acting on the tibial nerve in the tarsal tunnel. Hip flexion in the SLRTIBIAL test increased strain and excursion of the tibial nerve around the ankle about two-thirds that of the strain created by ankle dorsiflexion.
The investigators determined that the addition of hip flexion has no effect on the plantar fascia, but it does on the tibial nerve. They stated: "The cumulative effect of ankle dorsiflexion and hip flexion on strain in the tibial nerve in the tarsal tunnel demonstrates that elongation of a larger segment of the nerve bedding places larger mechanical forces on the tibial nerve in the tarsal tunnel than ankle dorsiflexion alone."
Butler examines the tibial nerve by putting pressure or tapping the tibial nerve by the malleolus to see if it radiates along the tibial track.4 If the medial plantar nerve is involved, a neural response may occur in the big toe. He uses the SLRTIBIAL test and adds pronation of the foot to stress the LPN, and uses abduction and pronation to stress the MPN. He exerts more tension to both of these areas by dorsiflexing the toes, and abducts the heel further to place more tension on the calcaneal branch.
To determine if a heel spur is causing local pain, put pressure on the local spur area. Hold this pressure and do an SLRTIBIAL test. If there is a neural response, the pain will alter compared to the local spur pain. Butler treats the tibial nerve by attempting to gradually mobilize its neuronal attachments. He might start with gentle ranges of motion out of tension, such as ankle dorsiflexion in knee and hip flexion. He then progresses to greater tension with the SLR with the foot in dorsiflexion and eversion, adding hip abduction and lateral rotation. Repetitive stretching to create neural mobilization is used.
In the office and at home, neural mobilization may be used during the slump position. The sitting patient flexes the neck and back with the ankle positioned into end-range dorsiflexion and eversion. The patient then extends the leg to apply more tension to the tibial nerve. The clinician can hold this foot position as the patient extends the leg.5
Stretching the gastrocsoleus complex, Achilles tendon, foot muscles such as the abductor halucis and quadratus plantae, correcting pronation, and strengthening weak areas are important. Techniques such as ART and Graston Technique should be beneficial to all related areas.
References
- Mann RA. Entrapment Neuropathies of the Foot. In: Orthopaedic Sports Medicine Vol. 2, 2nd. ed. DeLee JC, Drez D, Eds. Philadelphia: Saunders, 2003:2474-82.
- Alshami AM, Souvlis T, Coppieters MW. A review of plantar heel pain of neural origin: differential diagnosis and management. Manual Therapy, 2008;13:103-11.
- Coppieters MW, Alshami AM, Babri AS, et al. Strain and excursion of the sciatic, tibial and plantar nerves during a modified straight leg raising test. J Orthop Res, 2006;24(9):1883-9.
- Butler DS. Mobilization of the Nervous System. New York: Churchill-Livingston, 1991:213-30.
- Meyer J, Kulig K, Landel R. Differential diagnosis and treatment of subcalcaneal heel pain: a case report. J Orthop Sports Phys Ther, 2002;32(3):114-22.



