The proposed merger of the National Board of Chiropractic Examiners and Federation of Chiropractic Licensing Boards was approved by NBCE delegates and FCLB members at their respective annual meetings, held jointly in Atlanta, Ga., this year. Per the new bylaws, the new entity takes the NBCE name, with FCLB continuing as a department within NBCE. The federation will continue to enjoy Board of Directors representation on what will be a single, expanded board.
| Digital ExclusiveLoss of Internal Rotation
A motion deficit in all joints should be considered pathological. It appears, however, that loss of internal rotation in the shoulder and hip is related to more pathology than most other joints. The loss of internal rotation in shoulders, especially for baseball pitchers, has received significant study, but internal rotation loss for the shoulder and hip is also extremely important for the average patient.
Of course, even with the retroversion and adaptive remodeling of the tissues, symptoms or injury may occur if the forces or stresses about the glenohumeral joint exceed the range of load acceptance.1 Symptoms in the skeletally immature patient may be due to physeal injury. In the skeletally mature patient, symptoms and injuries are often due to boney stress reactions, anterior capsulolabral laxity and eventual instability. Osbahr, et al., in evaluating the throwing shoulder of college baseball players, speculated that complaints of pain from the proximal physis of the humerus may have stemmed from when the athletes were skeletally immature, before their college baseball pitching careers began.1 Their pain could therefore be osseous in origin, while tendinous pain might not have subsided. Humeral osseous retroversion may be demonstrated by a single radiograph.1,3
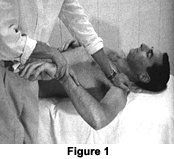
An important cause of GIRD is posterior capsule tightness. When the posterior capsule is tight, during external rotation, the humeral head translates more anteriorly than normal and is associated with the development of shoulder instability. With a tight posterior capsule during shoulder external rotation, there also can be stress to the posterior rotator cuff as the humeral head translates anteriorly. A significant limitation of internal rotation and posterior capsule tightness has been found to be associated with instability and impingement. Stretching of the posterior capsule and treatment of the posterior capsule using ART and Graston technique has clinically proven to solve this problem. Figure 1 depicts how to examine for range of internal rotation on a supine patient, with the examiner stabilizing the shoulder and scapula in 90 degree abduction while pushing down on the distal forearm. There should be at least 70 degrees of internal rotation.
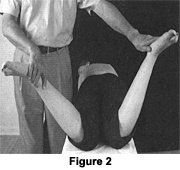
Hip evaluation of range of motion demonstrating a loss of internal rotation is always significant. Figure 2 depicts a prone patient with comparison of internal rotation for the hip. The right hip is limited. Limited, painful, internal hip rotation is found in internal derangements: slipped capital femoral epiphysis; muscular contracture (shortness of external hip rotators); sprain or partial rupture of the ischiofemoral ligament or the descending medial part of the iliofemoral ligament; hip bursitis (trochanteric, iliopectineal); or upper rectus tendonitis.4
Almost every hip osteoarthritis is associated primarily with decreased internal hip rotation, followed by reduced hip flexion.5 Loss of hip medial rotation with a hard end-feel is the first sign of osteoarthritis, followed by loss of hip flexion. As we age, the hip capsule becomes fibrotic and, because of the spiral arrangement of its fibers, taut, especially in medial rotation.
This pattern of limited passive motion is due to the capsular pattern of the hip, as described by Dr. Cyriax. The capsular pattern for most of the joints of the body that demonstrate a tight capsule (arthritis, arthrosis) or inflamed synovial tissue was established by Dr. Cyriax. The literature has agreed with most of his ideas regarding this concept over the past 50 to 60 years.4
References
- Osbahr DC, Dannon DL, Speer KP. Retroversion of the humerus in the throwing shoulder of college baseball pitchers. Am J Sports Med, 2002;30(3):347-353.
- Lintner D, Mayol M, Uzodinma O, et al. Glenohumeral internal rotation deficits in professional pitchers enrolled in an internal rotation stretching program. Am J Sports Med, 2007;35(4):617-21.
- Soderlund V, Kronberg M, Brostrom LA. Radiologic assessment of humeral head retroversion. Description of a new method. Acta Radiol, 1989;30(5):501-5.
- Hammer W. Functional Soft Tissue Examination & Treatment by Manual Methods, 3rd ed. Sudbury, Mass.: Jones & Bartlett, 2007.
- Altman R, Alarcon G, Appelrouth D, et al. The American College of Rheumatology criteria for the classification and reporting of osteoarthritis of the hip. Arthritis Rheum, 1991;34(5):505-14.



