A historic meeting between chiropractic and Make America Healthy Again (MAHA) leadership took place on March 10th, 2026, in Washington, D.C., featuring representatives from chiropractic national organizations, professional associations and policy principals. The collective goal: advancing the role of chiropractic in improving the health of Americans. Meeting participants focused on long-standing issues that have affected the chiropractic profession for decades, including access to care, reimbursement parity, and ensuring DCs have an appropriate role in national health policy discussions.
| Digital ExclusiveUpper Crossed Syndrome and Shoulder Pain
One of the most common injuries to afflict athletes of any skill level is shoulder pain. From the "weekend warrior" to the professional athlete, to the average fitness buff getting into shape; no one is immune to injury. Beyond obvious traumatic onset, very few clinicians understand the mechanism for acute shoulder injury and chronic pain. The majority of shoulder problems develop from microtraumatic events occurring due to poor joint biomechanics and muscular movement imbalances. It is important for the clinician to be aware that shoulder pain is usually a symptom of deeper problems that, unless corrected, may lead to total functional impairment.
Clinical Perspective
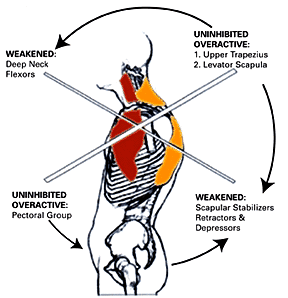
UCS leads to a forward head posture causing strain to the muscular attachments of the shoulder and shoulder blade. An anterior tilt and abduction ("flaring out") of the shoulder blades occurs, producing a rounded shoulder appearance. Due to the rounded shoulder posture, the mechanical axis of rotation of the glenoid fossa (shoulder socket) becomes altered. The humerus (arm) now requires additional stabilization from muscles that typically are quiet: the levator scapulae, upper trapezius, subscapularis, pectoralis minor and supraspinatus muscles. Postural overdevelopment of these muscles creates a deltoid shear (crossing of rotator cuff under AC joint), leading to shoulder impingement, tendonitis and bursitis syndromes.
Proper rehabilitation of the shoulder must include protocol for reversing the upper crossed syndrome. So, how do you do that? I have found the following program to be the most effective form of rehabilitation treatment.
Treatment Protocol
Due to chronic shortening, tightness and weakness in the primary stabilizers of the shoulder (supraspinatus, infraspinatus, teres minor and subscapularis), muscular adhesions and trigger points develop that must be removed before active/passive stretching. Failure to do so will result in stretch-reflex reciprocal inhibition and increased loss of muscle tone. Performing four to six sessions of myofascial release and trigger-point therapy usually is sufficient. Check all muscles in the UCS chart above. The most commonly affected muscles are the scalenes, pectoralis minor, infraspinatus and subscapularis.
Here are other aspects of this treatment protocol.
- Ultrasound the infraspinatus or subscapularis, depending on the most painful area of palpation and trigger-point referral pattern. Laser therapy also may be used. Typical dose is 170 Joules per point.
- Shoulder-blade retraction exercises for building the serratus anterior/posterior, trapezius and rhomboids, and for restoring scapular stabilization strength.
- Rotator cuff protocol: External rotation (three sets of 12-15 repetitions). Internal rotation not recommended due to the tendency of the subscapularis to become tight and overdeveloped.
- Y,T,W,L exercises on the stability ball to restore and enhance muscular recruitment patterns.
- Manipulation of the 5th and 6th cervical vertebrae and upper thoracics. Check the first rib for superior elevation, which can cause faulty AC joint mechanics, impingement syndrome and unrelenting trapezius muscle spasm.
- At-home treatment consists of rest and TENS to control pain. The tennis ball massage technique on the trapezius and infraspinatus (five to seven times per day) is extremely beneficial for breaking up active/latent trigger points. Self myofascial release with foam rollers on the upper back, lower latissimus dorsi, teres major/minor and infraspinatus will accelerate healing.
Most patients will be asymptomatic by the sixth visit and will demonstrate significant improvement in functional performance. The length of time it took to develop the problem is an indicator of how long you will need to work on correcting the faults before results will be felt. Don't forget that pain is often only the tip of the iceberg, directing you to the real underlying problem: upper crossed syndrome.



