A historic meeting between chiropractic and Make America Healthy Again (MAHA) leadership took place on March 10th, 2026, in Washington, D.C., featuring representatives from chiropractic national organizations, professional associations and policy principals. The collective goal: advancing the role of chiropractic in improving the health of Americans. Meeting participants focused on long-standing issues that have affected the chiropractic profession for decades, including access to care, reimbursement parity, and ensuring DCs have an appropriate role in national health policy discussions.
| Digital ExclusiveSacroiliac Instability: An Overview
Over the years, I have noticed that the most difficult sacroiliac (SI) patients have hypermobility, either obvious or hidden. If a joint is hypermobile, traditional chiropractic adjusting (high-velocity, low-amplitude) is not likely to help in the long term, even though these patients are "easy to adjust" and may get a few hours or a day of relief. The typical pattern is that they get relief from adjusting, but never hold the adjustment. Another scenario: Patients get relief and feel better, but then trivial trauma, a sudden twist or sitting too long, throws the SI off again, and they return with a recurrence of their low back and/or leg pain.
I have been writing about various aspects of the sacroiliac for a long time. This article is an overview or review. To utilize it best, visit http://marchellerdc.com/sacro-iliac.htm; you'll find many of the other articles I've written on SI over the years, including those referenced at the end of this article. You can also visit my columnist page (www.chiroweb.com/columnist/heller) and type in "sacroiliac" in the search box. I will share a couple of useful pieces directly in this article, including my favorite physical exam test for instability and the basic principle - compression - to use for adjusting an unstable SI.
Assessment
How do you determine that the joint is unstable? What you want to see is the preponderance of the evidence: several signs that together give you this indication. You can get this from a classic history (improved low back pain from manipulation, but the relief is short lived; and if the condition is recurrent). Women whose lower back pain started in pregnancy or at birth often have SI instability. You can start to suspect instability based on a global exam for laxity. Check range of motion at their thumbs and wrists, and see if they have an overall pattern of hypermobility, which will tend to lead to ligament problems in the SI. You can deeply palpate on the side of the ilium, where the gluteus medius posterior and gluteus maximus fibers originate, and may find exquisite tenderness here. You can deeply palpate the ligaments of the SI region, including the sacrotuberous, the long sacroiliac, and the interosseous SI ligaments, as well as the iliolumbar ligaments. When these are tender, they usually indicate SI hypermobility.
As you get better at palpating for instability, you will begin to notice a qualitative difference in lax or damaged ligaments: a lack of tone. You can motion test or spring the joint, testing for excessive mobility. I've illustrated my favorite test for this below. For this supine test, use your whole body, shifting toward the patient's feet, using the leverage of the patient's bent knee to open the joint.

I like this test as it levers open the SI joint, and after you've tried it on a few patients, you will appreciate the difference between the feel of a normal or fixated joint, and the feel of a hypermobile joint. If you just apply prone posterior to anterior pressure over the SI, you can easily get fooled. The body attempts to compensate for the hypermobility by tightening every possible structure that it can. I missed SI hypermobility almost completely for the first 12 years of my chiropractic career. You cannot find something you are not looking for.
There are a series of procedures that need to be done to stabilize a chronic, unstable, hypermobile SI joint. I'll outline them here, providing links to other articles I've written on these methods.
Manipulation
If the joint is hypermobile, high-velocity low-amplitude manipulation doesn't make a lot of sense. You are moving an already hypermobile joint. It is possible that the opposite SI is hypomobile. The osteopaths divide their methods into iliosacral and sacroiliac manipulations; I think this makes sense. Get the iliosacral joint lined up properly and then address the sacrum. (A few years back, I wrote a series of three articles about low-force iliosacral manipulation.1-3)
Conceptually, if the joint is unstable and separated, you need to think in terms of compression adjustments. Charles Blum, author of "Sacro-Occipital Technique's 'Category Two': A Remedy for Fixated Thinking," featured in the Sept. 1 issue of Dynamic Chiropractic,4 acknowledged this in reviewing the SOT model for category 2 and explaining the use of the SOT blocks. I've illustrated a prone way to correct the SI with compression below. You can use many different methods aimed at compression - aimed at closing the joint. You can use recoil or engage, listen, follow (ELF), counter-strain technique (done prone, bringing the leg into extension), or side-posture adjusting in the direction of compression.
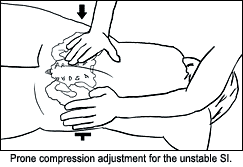
For the sacrum, you can visualize it as a problem in relation to the ilium or L5; you can visualize it as an intraosseous restriction.5 The key is that the sacrum should not feel rigid, stuck and tender. Your low-force manipulation should result in a better alignment and a better "feel" to the sacrum. Typically, a small area of the sacrum, left or right, and at a particular level, will feel most stuck.
Don't forget lumbar facet joints and midline lumbar compression issues, as well as the rest of the spine. In the lower extremity, consider the hip joints, knees, ankles and feet. Another significant area is the lower abdomen. Post-surgical scar tissue and visceral mobility issues can affect the SI region.6
Exercise
The most critical and most basic rehabilitation tool is establishing core stability. The basic tests of the core, such as variations on the active straight-leg-raise test, assess whether there is excessive SI motion on recruitment of the core muscles. The concept here is simple: If the patient fails these tests, their pelvis is moving incorrectly and they are continually re-injuring themselves doing the most basic, everyday motions of their body.7 This concept is the essence of force closure. Are the main stabilizing muscles doing their job? If you can enroll the patient in this process, they will have an excellent chance of success. If you cannot get the patient to pay attention, or if you don't know how to teach core stabilization, your odds of success diminish rapidly.
I like to teach my patients basic SI self-correction exercises.8 I think of these as self-mobilization movements. They really are not for a specific muscle, but are a valuable tool for the patient.
I am always trying to find what exercises give the patient relief. For some SI patients, it may be one of the piriformis stretches; for others, the SI self-correction; for others, a simple five-minute walk. Other muscles around the pelvis also can play significant roles. The gluteus medius and maximus, the hamstrings and quadriceps can need attention.
Is the patient sedentary? I like to recommend a basic pedometer and see how many steps they are taking in a day. A goal of 10,000 steps a day is great, but if they sit for eight hours a day, this may be hard to achieve. Walking is one of the best exercises for the SI. Sitting in a car for a long journey, especially without frequent breaks, is one of the worst insults to the SI.
Ligaments, Tendons, Muscles
When a joint is chronically unstable, there will be some degree of localized ligamentous laxity, some amount of insertional tendonopathy. If you do not address these issues, the muscles will work overtime and the joint will re-subluxate, as its primary support mechanisms are not doing their job. I know of two basic methods that address this, and I detailed this concept and treatment in a recent article.9 These methods include prolotherapy and frictional massage. I find instrument-assisted friction massage (e.g., Graston technique) to be faster and more effective, and it has some good research behind it. I think addressing these ligament and tendon issues is critical. Initiating first-stage healing is critical. Adjustments and exercise are not sufficient for this issue. See Warren Hammer's articles on tendonosis for a deeper understanding of this.10
Myofascial work can also be necessary on the involved muscles. This is a qualitatively different modality than instrument-assisted frictional massage. Myofascial work re-educates the tissue on a different level. If you do this yourself, great. If you don't, find a good massage therapist to work with.
Orthopedic Support
It is important that the unstable joint heal in the proper position and not constantly slip. Core stability, proper low-force adjustments, addressing ligaments and tendons, and teaching SI self-correction all contribute to this. Proper upright sitting, with a good chair and good back support, are essential. Beyond these, the patient usually needs an SI belt, also known as a trochanter belt. These are nonelastic or minimally elastic, and are worn down low, just above the greater trochanter of the hip. If the patient has pain on flexion, I'll put a belt on them in the office and then have them bend forward to see if the pain on flexion is reduced. Some authors state that overweight people have trouble with these belts, as they cannot get enough compression through the adipose tissue. Another important orthopedic support can be foot orthotics. If the foot is pronating with every step, this creates a torque up through the knees, hips and pelvis. Is the patient standing on concrete all day? Do they get any significant walking or sitting breaks? They may need to lie down for 5-10 minutes a few times a day to unload the joint completely.
Other Significant Factors
Consider mineral supplementation, especially magnesium, as mineral-deficient muscles cannot relax. An overall pro-inflammatory state, due to lack of omega-3s and the typical American diet, certainly impedes healing.
If I was limited to four things to do for a chronic SI, I would start with core stability training, have the patient wear an SI belt, perform instrument-assisted frictional massage, and provide the correct adjustments.
This article is a 12,000 word opus, compressed into 1,700 words. I have tried to be comprehensive, and yet I know there are other factors to discuss, depending on the patient. Stress plays a role in all illness. I am always looking for what I am missing when the patient doesn't get well reasonably quickly. I hope I have given you some ideas to look beyond your usual assessment and treatment tools for the chronic SI patient.
References
- "Iliosacral Diagnosis and Treatment, Part One." Dynamic Chiropractic, Jan. 27, 2003. www.chiroweb.com/archives/21/03/08.html.
- "Iliosacral Diagnosis and Treatment, Part Two." Dynamic Chiropractic, March 10, 2003. www.chiroweb.com/archives/21/06/06.html.
- "Iliosacral Diagnosis and Treatment, Part Three." Dynamic Chiropractic, April 21, 2003. www.chiroweb.com/archives/21/09/15.html.
- "Sacro-Occipital Technique's 'Category Two': A Remedy for Fixated Thinking." Dynamic Chiropractic, Sept. 1, 2006. www.chiroweb.com/archives/24/18/08.html.
- "The Sacrum." Dynamic Chiropractic, July 14, 2003. www.chiroweb.com/archives/21/15/08.html.
- "Abnormal Scars as a Cause of Myofascial Pain." Dynamic Chiropractic, Nov. 30, 2004. www.chiroweb.com/archives/22/25/14.html.
- "Assessing Core Stability: Basic Evaluation, Basic Exercises." Dynamic Chiropractic, March 12, 2006. www.chiroweb.com/archives/24/06/11.html.
- "Sacroiliac Joint Correction - A Different Model." Dynamic Chiropractic, Dec. 17, 2005. www.chiroweb.com/archives/23/26/09.html.
- "Sacroiliac Revisited: The Importance of Ligamentous Integrity." Dynamic Chiropractic, July 2, 2005. www.chiroweb.com/archives/23/14/10.html.
- See www.chiroweb.com/columnist/hammer (type "Tendonosis" in the search box) or www.warrenhammer.com/articles_main.htm.



