The proposed merger of the National Board of Chiropractic Examiners and Federation of Chiropractic Licensing Boards was approved by NBCE delegates and FCLB members at their respective annual meetings, held jointly in Atlanta, Ga., this year. Per the new bylaws, the new entity takes the NBCE name, with FCLB continuing as a department within NBCE. The federation will continue to enjoy Board of Directors representation on what will be a single, expanded board.
| Digital ExclusiveHamstring Tidbits
A common problem with hamstring injuries is their tendency to recur. While the cause of hamstring injuries is considered multifactorial, it is difficult to identify the factor or combination of factors responsible for strain recurrence.1 Considering the muscle's high percentage of fast-twitch type II fibers, hamstring injuries usually occur during of the swing phase of gait (decelerating hip flexion and knee extension). The biceps femoris is the part of the hamstring most often injured.
The hamstring, especially the biceps femoris, essentially is attached to the skull, since it fascially attaches to the sacrotuberous ligament, across the sacrum to the thoracolumbar fascia (TLF). The TLF attaches to the latissimus dorsi, transverses abdominus, internal obliques and rhomboids to the splenius capitis and cervicus tendons to the occiput. It is apparent, therefore, that the hamstrings connect to the lumbar-pelvic spine, upper torso, shoulder and skull.2,3
TFL tensions can be transmitted to the SIJ from its deep fibers, which connect to the sacrotuberous ligament, generating forces perpendicular to the SIJ.4,5 Therefore, it may be possible that the TFL, acting as a back extensor retinaculum, aids in lumbar-pelvic stability. It has been found that with delayed activation of the transverses abdominus, hamstring tension can tighten the TLF and help stabilize the sacroiliac joint (SIJ).4,5 If there is delayed activation of the transverses abdominus, there also may be earlier contraction of the biceps femoris to compensate for the weak TFL system, putting the hamstring at a disadvantage. The back and pelvis should therefore be evaluated, especially when there is a recurrent hamstring strain. Although the above information relating the lumbar pelvic mechanism to the hamstrings appears empirically valid, at present, there are very few studies to prove that improving the mechanics of the lumbar-pelvic and its relationship to body posture, pelvic tilt, leg length and scoliosis will prevent hamstring strains.5 As usual, definitive research is needed.
By increasing the amount of anaerobic interval training, stretching while the muscle is fatigued, and implementing sport-specific training drills among Australian soccer players, G. M. Verrall, et al.,6 saw a significant reduction in the number and consequences of hamstring muscle strain injuries among the athletes. In the laboratory, fatigued muscles are able to absorb less energy when undergoing stretching, thus making them more vulnerable to injury when compared to non-fatigued muscles. Therefore, improving fatigue resistance in muscle should fatigue resistance in muscle should help prevent muscle strain injury. The researchers felt that stretching could have a role in hamstring muscle strain injury prevention by improving force absorption for a given length of muscle, thereby making the muscle more resistant to stretch injury. The stretches were perfomed at a time when it was considered that the muscle would be fatigued, in order to develop increased fatigue resistance of the hamstring muscle. The researchers also wanted to induce a change in the viscoelastic properties of muscle so as to increase energy absorption and decrease load on the muscle-tendon unit for any given length, especially in body positions of function and vulnerability to injury.
In a classic study by Taylor, et al.,7 they attempted to prove that muscle response to stretch was based more on the muscle's viscoelastic properties, rather than on reflex effects of PNF techniques such as contract-relax exercises. While stretching involves an active component, as in PNF methods, the passive component resides mostly in the connective tissue of the muscle-tendon unit. Muscle tendons are viscoelastic tissues; when stretched and held at a constant length, the stress at that length gradually declines - this is "stress relaxation." "The behavior of the material is both viscous, because the tension decreases with time, and elastic, because the specimen maintains some degree of tension."7 "Creep" is a good example.
PNF techniques work by inducing stress relaxation by applying tension to the viscoelastic elements during passive stretch and active isometric contraction. Taylor, et al., proved that the viscoelastic properties were more important than the reflex theory by showing that denervated muscles responded similarly to the innervated muscles; they decided there were no significant force contributions from a stretch reflex.
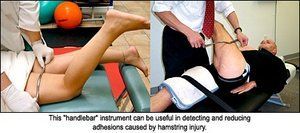
A probable cause of recurring hamstring injury also might be the inability to adequately assess and treat the severity of the initial damage, resulting in premature return to competition at a time in which the injury is still in the remodeling phase of inflammation and repair. The initial treatment may not have removed the scar tissue and adhesions that accumulated, predisposing the muscle to re-injury.5 Soft-tissue techniques such as active release, neuromuscular rehabilitation, friction massage and Graston technique (GT) can be very effective in reducing adhesions. I especially like the GT instrument called the "handlebar" (see images above), which can be used to detect and eliminate adhesions.
References
- Croisier JL. Factors associated with recurrent hamstring injuries. Sports Med 2004;34(10):681-695.
- Barker PJ, Briggs CA. Bogeski G. Tensile transmission across the lumbar fasciae in unembalmed cadavers: effects of tension to various muscular attachments. Spine 2004;29(2):129-38.
- Barker PJ, Briggs CA. Attachments of the posterior layer of lumbar fascia. Spine 1999;24(17):1757-64.
- Vleeming A, Stoeckart R, Sniders VJ. The sacrotuberous ligament: a conceptual approach to its dynamic role in stabilizing the sacroiliac joint. Clinical Biomechanics 1989a;4:201-3.
- Hoskins W, Pollard H. The management of hamstring injury. Part 1: issues in diagnosis. Manual Therapy 2005;10:96-107.
- Verrall GM, Slavotinek JP, Barnes PG. The effect of sports specific training on reducing the incidence of hamstring injuries in professional Australian Rules football players. Br J Sports Med 2005;39:363-368.
- Taylor DC, Dalton JD, Seaber AV, Garrett WE. Viscoelastic properties of muscle-tendon units: the biomechanical effects of stretching. Amer J Sports Med 1990;18(3):300-309.



