The proposed merger of the National Board of Chiropractic Examiners and Federation of Chiropractic Licensing Boards was approved by NBCE delegates and FCLB members at their respective annual meetings, held jointly in Atlanta, Ga., this year. Per the new bylaws, the new entity takes the NBCE name, with FCLB continuing as a department within NBCE. The federation will continue to enjoy Board of Directors representation on what will be a single, expanded board.
| Digital ExclusiveA Three-Step Program for Chronic Low Back Pain
In many cases of chronic low back pain, early and aggressive treatment produces optimum results for the patient. I have found the following three-step approach highly effective: spinal manipulation of the lumbopelvic area, along with the adjunctive therapies of rehabilitative exercise and external supports.
Step 1: Spinal Manipulation
A "two-to-three-week regimen of daily spinal manipulations by an experienced chiropractor" brought significant improvement in 81 percent of totally disabled patients with chronic low back and referred leg pain, as reported in a study by Kirkaldy-Willis and Cassidy.1 The 238 subjects in this study were from a university back pain clinic for patients who had failed to respond to previous conservative or surgical treatment. The researchers stated: "In our experience, anything less than two weeks of daily manipulation is inadequate for chronic back pain patients".1
Achieving success requires selecting a spinal adjusting procedure which will best assist the patient in regaining lumbopelvic structural function and alignment. The treatment methods which brought about such excellent results are easily reproduced by most chiropractors. Cassidy and Mierau report that they used specific "side-posture manipulation of only the fixed or dysfunctional lumbar posterior joints or sacroiliac joints. A high-velocity, low-amplitude thrust was employed to the target joint after careful positioning and relaxation of the patient."2 Motion palpation of the lumbosacral region was used to identify the target joint which required adjustment.3 Research has shown this approach to be effective even when there is evidence of a spondylolisthesis (the segments above and below the slipped vertebra are targeted)2 or a herniated disc.4
Step 2: Rehabilitative Exercises
The muscles of the torso and pelvis play an important role in providing support and stability to the lumbar spine, similar to guy wires supporting a telephone pole.5 Involving the patient in an appropriate low back exercise program has been found to be very beneficial,6 even in herniated disc cases.7 Flexibility and strength exercises can bring about rapid improvements in lumbar spinal function and decreases in pain levels.8
Specific exercises must develop "dynamic control of lumbar spine forces to eliminate repetitive injury to the intervertebral discs, facet joints, and related structures."9 Recommending specific exercise(s) is not always clear-cut: some research supports the need for abdominal strengthening,10,11 other studies advise pelvic tilts,12 and still other reports focus on the importance of strengthening the lumbar extensor muscles.13,14
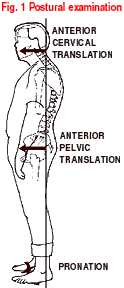
The needs of patients vary. The exercises that worked for one will not necessarily work for another. However, the first step toward a solution is to use clinical testing (Goldthwait's and Gaenslen's tests are good starting points) and postural evaluation (see Figure 1) to identify the most appropriate and effective lumbopelvic exercise routine(s).

The "mirror image" concept of postural examination and rehabilitation15,16 is an accurate and very easy method of determining which primary exercise is most important. By evaluating the patient's three-dimensional posture in a reference frame and noting any specific deviations from the ideal intrinsic equilibrium, the doctor is able to identify the sources of excessive biomechanical stress and give specific corrective exercise recommendations (see Figure 2). A general conditioning and flexibility program will complement the specific corrective postural exercises.
Step 3: External Supports
The use of external supports to reduce excessive biomechanical forces on the lumbar spine is a significant treatment approach, it is one which is frequently overlooked by practitioners. Postural supports for sitting (postural back rests or ischial lifts for chairs and car seats), standing (such as custom foot orthotics and heel lifts) and sleeping (mattresses and pillows) can greatly assist in the management of lumbar spine conditions.
As McKenzie states, "A poor sitting posture will frequently enhance and always perpetuate the problems in patients suffering from low back pain." He goes on to recommend the use of a back rest support to help maintain the lumbar lordosis and prevent sitting strain.17
During standing and walking (not to mention running in athletes), the lumbar spine and pelvis balance on the lower extremities. If leg or foot asymmetries or alignment problems are present, abnormal forces are transmitted along the closed kinetic/kinematic chain, interfering with spinal function.18 When excessive pronation and/or arch collapse is present, a torque force produces internal rotation stresses to the leg, hip and pelvis.19
These forces can be decreased significantly with the use of custom-made, corrective orthotics. In patients with degenerative changes in the lumbar discs and facets, the external force of heel strike may aggravate and perpetuate low back pain. This force can be easily reduced with the use of shock-absorbing soe inserts20,21 or orthotics which contain viscoelastic compounds. An anatomical difference in leg length produces abnormal structural strains on the pelvis and low back. Such strains can cause not only chronic pain22,23 but have also been shown to result in specific degenerative changes.24 The use of an orthotic and/or heel lift has been shown to reduce these structural strains and bring about significant clinical response.25,26
Sleep postures can also have a detrimental effect on the structural stability of the lumbar spine. While most experts recommend a firm mattress, McKenzie also suggests the use of a "sleeping roll" to maintain proper lumbar positioning during sleep.27 Regarding waterbeds, a research study of chronic low back pain patients compared four different types of beds and found that a hard "orthopedic"-type bed was best.28
References
- Kirkaldy-Willis WH, Cassidy JD. Spinal manipulation in the treatment of low back pain. Can Fam Phys 1985;31:528-40.
- Mierau D, Cassidy JD, et al. A comparison of the effectiveness of spinal manipulative therapy for low back pain patients with and without spondylolisthesis. J Manip Physiol Ther 1987;10:49-55.
- Cassidy JD, Potter GE. Motion examination of the lumbar spine. J Manip Physiol Ther 1979;2:151-8.
- Cassidy JD, Thiel HW, Kirkaldy-Wills WH. Side posture manipulation for lumbar intervertebral disk herniation. J Manip Physiol Ther 1993;16:97-103.
- Farfan HF. The biomechanical advantage of lordosis and hip extension for upright activity. Spine 1978;3:336-42.
- Mayer TG, Gatchell RJ, et al. Objective assessment of spine function following industrial injury: a prospective study with comparison group and one-year followup. Spine 1985;10:482-93.
- Saal JA, Saal JS. Nonoperative treatment of herniated lumbar intervertebral disc with radiculopathy: an outcome study. Spine 1989;14:431-7.
- White AA, Panjabi MM. Clinical Biomechanics of the Spine, 2nd ed. Philadelphia: J.B. Lippincott, 1990:429.
- Saal JA, Saal JS. Rehabilitation of the patient. In: White AH, Anderson R. (eds.) Conservative Care of Low Back Pain. Baltimore: Williams & Wilkins, 1991:31.
- Williams PC. Lesions of the lumbosacral spine: chronic traumatic (postural) destruction of the lumbosacral intervertebral disc. J Bone Joint Surg 1937;19:690.
- Schmidt GL, Herring T, et al. Assessment of abdominal and back extensor functions. Spine 1983;11:19-27.
- Partridge MJ, Walters CE. Participation of the abdominal muscles in various movements of the trunk in man: an EMG study. Phys Ther Rev 1959;39:791-800.
- Mayer TG, Smith SS, et al. Quantification of lumbar function: sagittal plane trunk strength in chronic low-back pain patients. Spine 1985;10:765-72.
- Beinborn DS, Morrissey MC. A review of the literature related to trunk muscle performance. Spine 1988;13:655-60.
- Harrison DD. Chiropractic: The Physics of Spinal Correction. CBP Technique, 1992.
- Christensen KD, et al. Postural rehabilitation guidelines. In: Chiropractic Rehabilitation Association's Rehabilitation Guidelines for Chiropractic, 1st ed. Ridgefield, WA: CRA, 1992:5-10.
- McKenzie RA. The Lumbar Spine: Mechanical Diagnosis and Therapy. Lower Hutt, NZ: Spinal Pubs, Inc., 1981:4,87.
- Keane GP. Back pain complicated by an associated disability. In: White AH, Anderson R. (eds.) Conservative Care of Low Back Pain. Baltimore: Williams & Wilkins, 1991:307.
- Hammer WI. Hyperpronation: causes and effects. Chiro Sports Med 1992;6:97-101.
- Light LH, et al. Skeletal transients on heel strike in normal walking with different footwear. J Biomechanics 1980;13:477-80.
- Fauno P, et al. Soreness in lower extremities and back is reduced by use of shock absorbing heel inserts. Int J Sports Med 1993;14:288-290.
- Giles LGF, Taylor JR. Low-back pain associated with leg length inequality. Spine 1981;6:510-21.
- Friberg O. Clinical symptoms and biomechanics of lumbar spine and hip joint in leg length inequality. Spine 1983;8:643-51.
- Giles LGF, Taylor JR. Lumbar spine structural changes associated with leg length inequality. Spine 1982;7:159-162.
- Hoffman KS, Hoffman LL. Effects of adding sacral base leveling to osteopathic manipulative treatment of back pain: a pilot study. JAOA 1994;94:217-26.
- Yochum TR, Barry MS. The short leg (revised edition). Practical Research Studies 1994;4(5).
- McKenzie RA. The Lumbar Spine: Mechanical Diagnosis and Therapy. Lower Hutt, NZ: Spinal Pubs, Inc., 1981:4,92.
- Garfin SR, Pye SA. Bed design and its effect on chronic low back pain -- a limited controlled trial. Pain 1981;10:87-91.



