The proposed merger of the National Board of Chiropractic Examiners and Federation of Chiropractic Licensing Boards was approved by NBCE delegates and FCLB members at their respective annual meetings, held jointly in Atlanta, Ga., this year. Per the new bylaws, the new entity takes the NBCE name, with FCLB continuing as a department within NBCE. The federation will continue to enjoy Board of Directors representation on what will be a single, expanded board.
| Digital ExclusiveGuidelines for the Management of CAD Trauma - Use Them
Case I
Recently, I was in another state speaking for a private group of attorneys and a multidisciplinary health care audience. One of the DCs related a story to me. Without mentioning any names, it seems the DC's associate had been having difficulties with a now-defunct peer-review system. Specifically, when a provider was tagged by one of the DCs on this peer-review board as providing what they viewed as excessive care, overutilization, or other excess, the case would be sent to a branch of the attorney general's office and an investigation initiated.
I don't know whether the word "fraud" was used, but surely it was implied in this kind of thing. Apparently, records were seized, and for the next three years this hapless DC was squeezed through the emotional ringer as the lengthy investigation proceeded. Eventually, a plea bargain was proposed. The DC could cop to a lesser plea but his employer, the DC now telling me this story, wouldn't allow it. Essentially, we're talking about prosecuting the "crime" of treating a CAD patient about 70-some-odd times over a year or so - a treatment duration considered excessive by the peer review DC. This isn't an unusual case. I've heard many like it.
The owner DC hired a lawyer to handle the associate's case. Eventually they had the opportunity to depose this peer review DC. Noticing on his CV that he was a graduate of my whiplash certification program, the lawyer asked the DC about me. He conceded that he considered me an expert in CAD trauma. The hook was taken. He then asked the DC if he was aware that, in addition to pain and the physical findings of limitations of cervical spine motion, this patient also had neurological complaints. (Her neurological complaints were a major component of her condition and the complicating factor that necessitated her lengthy care.) The DC admitted that he was aware of the neurological complaints.
The attorney asked whether the DC would thus consider her injury a Grade III, alluding to the grading system that is now used universally to characterize whiplash/CAD trauma. He admitted that he would. The hook was set; the trap door sprung. Referring the DC to the guidelines published in my textbook1 and elsewhere (see Table I below), including the training manuals used at the program the DC had listed on his CV, the attorney asked if the treating DC had indeed been within the guidelines. The peer review DC paused and then admitted that the treatment was probably not excessive. After three long miserable years, the case was dropped.
Case II
Last year, under the strong leadership of Ron Tripp, DC, the Oklahoma State Board of Chiropractic Examiners adopted these guidelines for use in peer review disputes. (They have also been adopted by other states and associations.) Ron told me recently that when he is cross-examined in medicolegal situations about the length or frequency of care, he simply defers to the guidelines and finds this strategy to be essentially bombproof.
I imagine that the exuberant self-confidence characteristic of a former world heavyweight judo champion (which Ron is) doesn't hurt either, but the point I attempt to make here is simply this: We are all caught in a highly polarized health care system. Around every corner it seems we are being coerced into compromising our care and reducing our fees. The big business collective of insurers have their team of assimilated doctors whose job is to steer errant health care providers back onto what they perceive as the straight and narrow path of reasonable health care. But who decides what is reasonable? Is there really any question? These peer review physicians are all too often no more than loyal company lackeys programmed to churn out "boilerplate" reviews used as pretexts for denials of benefits - or worse, as in the above example. And, as in the example I gave above, published guidelines can be the treating physician's deliverance. Use them.
Case III
I testified in a trial in San Diego a few weeks ago involving a fairly high-speed crash. Liability was admitted. One of the critical issues in the case was the number of treatments provided by the patient's now-deceased DC. An orthopaedic surgeon performed an IME and concluded that 12 weeks of care should have been sufficient, and that anything beyond that was excessive.
During my direct examination, I explained to the jury that the patient had a Grade IV injury. I showed the jury a poster of these guidelines and how, with a Grade IV injury and so many other risk factors, the guidelines simply could not be applied to this patient. However, to the DC's credit, he had managed to treat a Grade IV injury within the Grade III guideline allowance. They apparently understood. The plaintiff prevailed in court.
Guideline Development
Where do these guidelines come from? A number of methods have been employed in the development of guidelines. At RAND we used the so-called delphi technique. A panel of experts from divergent fields analyzed the evidence for support of a treatment and ranked a large series of issues (for example, the appropriateness of cervical spine manipulation) accordingly.2 A somewhat less formal method is to invite a panel of experts to attend a meeting and come to a consensus on pre-selected topics. The results depend on the qualifications of the panelists. A good example of how such things can go wrong is the New Jersey case of a couple of years back.
The Banking and Insurance Commission (now there's an obvious concatenation) in New Jersey hired the accounting firm Pricewaterhouse Coopers to develop a set of "care paths," designed to act as guidelines for clinical practice. These algorithms were developed by a staff of non-experts, including RNs - even an MBA. They cited less than 20 scientific or clinical papers to support their findings. The depth of their befuddlement is illustrated by the fact that, while attempting to enlist the aid of the "Quebec Task Force on Whiplash-Associated Disorders" paper published in Spine in 19953 - one which promulgated guidelines based on faulty research methodology - they inadvertently cited the paper by Michael Freeman, myself, and Anne Rossignol criticizing the paper for those errors! Our paper was published in Spine in 1998,4 but the title contained the words "Quebec Task Force on Whiplash-Associated Disorders." It probably threw them off and, like most of the other cited literature, they probably didn't bother to read it.
The resulting "care paths" severely limited the amount of care available to whiplash patients from chiropractic physicians to just a handful of treatments. Make no mistake about it, these guidelines bear no relationship to actual practice norms, nor are they based on any scientific or academic work. Many other treatable conditions were dealt with, with similar careless and reckless disregard for science and public health. It was clearly a fait accompli for the BIC. And despite letters from myself, Michael Freeman, and even an appearance before the board by Scott Haldeman, the care paths were railroaded through the system at the expense of care providers and their patients, and served as a great pretext for denial of future claims.
According to a piece in the September 2000 issue of Smart Business Magazine, the Securities and Exchange Commission (Sec) reported that partners at the world's largest accounting firm routinely violated rules forbidding them from owning equity in companies they were auditing. "Thirty-one of Pricewaterhouse Coopers' 43 partners committed at least one violation, as did six of the 11 partners responsible for enforcing the investment and securities rules. The SEC probe uncovered 8,064 violations; five partners were dismissed in the aftermath." Hard to believe.
Another method of guideline development is to survey practices. That's how my guidelines were developed. A review of about 2,000 cases, graded as to severity (i.e., Grades I-V), provided the basis for these guidelines (see Table I). These were originally published in 1993.5 A few years later, the Insurance Research Council (IRC) reported that the average number of treatments provided by DCs in cases of CAD trauma was 32.6 Considering that most CAD injuries requiring treatment will be graded either Grade II or III, this serves to validate the guidelines to some degree. That the average number of treatments is 32 doesn't in any way imply that this is the best for which we can hope. It is quite likely that less than optimal care was provided in many cases, since many DCs - like their medical counterparts - are not well trained in treating these patients. Optimal treatment methods are something we should strive to discover through future research.
Table I
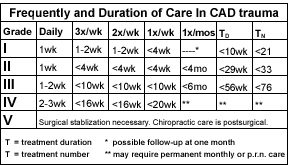
Conclusion
As certain as death and taxes are, we can also expect to be subjected to somebody's guidelines. While they are useful for health care providers to monitor and gradually improve treatment strategies, they also have utility for reimbursement policy.
In the vacuum of existing guidelines, we can be expected to submit to the whims and fancies of peer reviewers whose opinions are largely reflective of their employers' company policies and generally ungrounded in science. We can simply stand around with our hands in our pockets, hoping for the best, and taking our chances with the likes of Pricewaterhouse Coopers, or we can take a stand and support a policy that we consider to be in the best interests of our patients and our own welfare; one that is based upon sound clinical experience, practice norms, and the best scientific evidence available. Clearly, the latter choice is the only reasonable one.
The guidelines presented in this paper have been in our literature now for seven years and no competing guidelines have been published during that time, with the exception of the Quebec Task Force Guidelines,3 but these are applicable only for patients who are on disability (i.e., not at work or their usual activities). Use the guidelines presented here to support the need for care, but remember - they are only guidelines, not prescriptions for treatment. Guidelines assist physicians to better treat their patients and to compare their practices with their peers. The patient is the ultimate guide to care, with some recovering well before the allotted guideline period suggests. And others, due to other complicating factors such as advanced age, prior disease, etc., cannot be practically placed within such a guideline.
References
- Croft AC: Management of soft tissue injuries. In Foreman SM, Croft AC (eds), Whiplash Injuries: the Cervical Acceleration/Deceleration Syndrome,second edition, Baltimore, Williams & Wilkins, 1995, p 465.
- Coulter ID, Hurwitz EL, Adams AH, Meeker WC, Hansen DT, Mootz RD, Aker PD, Genovese BJ, Shekelle PG. The Appropriateness of Manipulation of the Cervical Spine. Santa Monica, RAND Corporation, 1996.
- Spitzer WO, Skovron ML, Salmi LR, Cassidy JD, Duranceau J, Suissa S, Zeiss E. Scientific monograph of the Quebec Task Force on whiplash-associated disorders: redefining 'whiplash' and its management. Spine (Supplement) 20(8S):1S-73S, 1995.
- Freeman MD, Croft AC, Rossignol AM: Whiplash associated disorders: redefining whiplash and its management. Quebec Task Force: a critical evaluation. Spine 23(9):1043-1049, 1998.
- Croft AC: Treatment paradigm for cervical acceleration/deceleration injuries (whiplash). ACA J Chiro 30(1):41-45, 1993.
- Paying for Auto Injuries: A Consumer Panel Survey of Auto Accident Victims. Insurance Research Council, May, 1994, p 9.
Arthur Croft,DC,MS,FACO,FACFE
Director, Spine Research Institute of San Diego
San Diego, California
drcroft@san.rr.com



