The proposed merger of the National Board of Chiropractic Examiners and Federation of Chiropractic Licensing Boards was approved by NBCE delegates and FCLB members at their respective annual meetings, held jointly in Atlanta, Ga., this year. Per the new bylaws, the new entity takes the NBCE name, with FCLB continuing as a department within NBCE. The federation will continue to enjoy Board of Directors representation on what will be a single, expanded board.
| Digital ExclusiveDetermining What Exercise to Prescribe
The Functional Approach as a Practical Tool
While restoring function can be an overwhelming task, the focus can be narrowed down to the primary goal of increasing the patient's functional range (FR). Initially, this consists of the painless or pain-centralizing activities revealed in the patient's history or range-of-motion examination. Orthopaedic, McKenzie, and myofascial evaluation are the first assessment approaches utilized to determine the FR. Once identified, it is invaluable in the clinic as an audit for pre-and posttesting of the patient's status, and as a guide to determining what treatment is most effective.
After finding the movements or positions that aggravate (peripheralize) or relieve (centralize) the patient's symptoms, it is important to identify the patient's major functional pathologies. This is usually a joint blockage or altered movement pattern (pathokinesiology) related to painful tissue, movement, or activity intolerance.
Thus, the limits of the patient's FR consist of the aggravating movements and positions, and the key functional pathology related to those symptoms. According to Dennis Morgan, a pioneer in spinal stabilization training,"the functional position is the most stable and asymptomatic position of the spine for the task at hand" (Morgan, 1988). Thus, before exercise can be prescribed, a thorough history and examination of the patient's mechanical sensitivities should be carried out (Vollowitz, 1988; McKenzie, 1987).
| To Identify the FR
|
Initial exercises are always carried out within the patient's FR. The exercises should be pain-centralizing or relieving (McKenzie/orthopaedic), and they should be performed with good stability or movement patterns (functional pathology).
McKenzie Principles - The Orthopaedic Approach to Acute Symptoms
The orthopaedic approach connotes the assessment and treatment of mechanical problems of the locomotor system. In the context of functional restoration, orthopaedic assessment specifically deals with identifying the movements and positions that are painful or painless. For example, Kemp's or Gaenslen's tests are positive if they reproduce the patient's characteristic pain. McKenzie has provided one of the best guides to exercise prescription in his description of centralization. According to his philosophy, clinicians should identify the positions and repetitive movements that increase, decrease, or centralize symptoms. The movements or positions that reduce symptoms, or centralize peripheral symptoms, can be recommended as self-treatment (McKenzie, 1987).
Both history and examination are involved in this analysis. For instance, the history should identify what positions or movements aggravate, relieve or are neutral to the patient's symptoms, in particular, peripheral symptoms. Sitting and forward-bending intolerances strongly suggest a disc problem, and self-treatment would be "biased" toward extension. Another example of the importance of a thorough history is that many patients explain that they are worse after sitting or standing for a prolonged period of time. Such postural findings are often the only clues when the examination cannot reproduce time-dependent mechanical sensitivities.
Clinical examination should include orthopaedic tests that seek out the movements or positions that provoke the patient's characteristic symptoms. McKenzie has added to this the use of repetitive tests of movements, such as those in the cardinal ROMs, in order to better simulate normal activities that are typically repetitious. In addition, the patient's own historical report of functional activities that aggravate symptoms can be confirmed by the examination of functional activities.
Clinical Utility of the McKenzie/Orthopaedic Examination
|
The movements and positions found to aggravate symptoms are used as an audit for pre and posttesting to assess the patient's progress. In contrast, the pain-centralizing or relieving positions and movement ranges are utilized for exercise training.
Myofascial Pain
If it is difficult to elicit a patient's characteristic pain with orthopedic or ROM tests (i.e., McKenzie postural syndrome), the myofascial examination becomes pivotal. If active trigger points can be found that reproduce the patient's characteristic pain, a sure-fire treatment guide is at hand, especially as a pre-and posttreatment re-check of patient response and status.
Identifying the Key Functional Pathologies Responsible for Pain or Activity Intolerances
The cause of 90 percent of spine pain is unknown. Therefore, most guidelines recommend use of the unsatisfactory label "nonspecific" back pain (Spitzer, 1987, AHCPR, 1994, DIHTA, 1999). Even though most back pain is called "nonspecific," it would be a mistake to assume that this pain is psychogenic or that there is no etiology or mechanism of injury. In fact, new research is pointing toward motor control deficits as the most promising candidates for playing an aetiopathologic role in spinal disorders (Mannion, et al., 2001; McGill, 2001, 2003, Radebold 2000, 2001, Cholewicki 2000).
Practice-Based Problem Patients often present with innumerable functional pathologies relating to poor motor control. Therefore, how can the "key link" or relevant dysfunctional chain be identified? |
The relevant functional pathologies are those related to the pain generator or injured tissue. This is primarily by being a source of biomechanical overload, which eventually leads to repetitive strain of the painful tissue (Kibler 1998). An example of this is a patient who presents with neck pain; the functional pathology responsible may be the head-forward posture and poor motor control of cervicocranial flexion. Another example would be a patient presenting with knee pain; the key functional pathology may be a kinetic chain dysfunction in which subtalar hyperpronation causes internal tibial rotation during gait or squatting.
One of the most relevant indicators of poor motor control is global muscle overactivity. This is one of the most clinically useful signs of dysfunction in the kinetic chain. According to Richardson, et al. (Richardson, 2000):
"In approaching treatment, the clinician must answer two basic questions:
Does the patient present with unwanted global muscle activity?
If so, which muscles are problematic?
These questions must be answered in order to institute best-practice therapeutic exercise."
| Clinical Utility of Identifying the Key Functional Pathology
|
In addition to what muscles are overactive, the question, "Why are they overactive?" is also pivotal. Global muscle overactivity is a sign of a dysfunctional kinetic chain, but it is not usually the cause of the dysfunction. Frequently, the key dysfunction is a blocked joint or weak muscle at some distance from the site of symptoms, or global muscle overactivity. Therefore, therapy begins with manipulation of a key dysfunctional tissue, such as a hypomobile joint, and then progresses to functional training of relevant movements without excessive global muscle substitution.
Clinical Examples
Two of the most clinically significant signs of global muscle overactivity are thoracolumbar hypertonus and head-forward posture with sternocleidomastoid (SCM) hypertonus.
Thoracolumbar hypertonus (Figure 1) is assessed during observation of:
- standing postural anaylsis;
- Janda's prone leg extension test; and
- Hodges' quadruped leg reach exercise.

Therapy may consist of treatment of a key joint, such as the thoracolumbar junction, and motor control training of the lumbar region involving the "deep" stabilizers. Examples include the quadruped leg reach or prone abdominal hollowing within functional range (i.e., without global muscle overactivity or periphera-lization of symptoms).
Head-forward posture with SCM overactivity (Figure 2) is assessed during observation of standing or seated postural analysis, and Jull's cervicocranial flexion test (Jull, 2000).
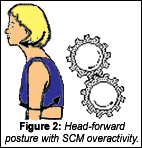
Motor control treatment of the cervicothoracic region involves "deep" stabilizer training, such as cervicocranial flexion (deep neck flexors without SCM substitution), or facilitation of the upper quarter "deep" stabilization chain (i.e., Brügger exercise for supinators, extensors, exteral rotators and abductos.)
These stabilization exercises should be coupled with appropriate chiropractic treatment (i.e., adjustments or manual therapy) to achieve the primary goals of reducing the patient's activity intolerances and increasing range of painless movements. Whenever possible, patients should be tested and trained in their functional activities (i.e., home, sport, and work). For instance, if a person engages in pushing or throwing activities, the following exercises should be integrated into their program (Figures 3, 4). Once again, these activities should be performed in the patients' FR.

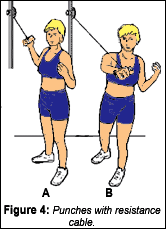
Two key questions must be answered prior to prescribing an exercise program for a patient with spinal pain: "What exercises are best tolerated by the individual patient?" and "What is the most relevant dysfunction responsible for specific activity intolerances?" This approach provides a simple filter that can be utilized to aid in the selection of the appropriate treatment.
Rehabilitation has achieved its goal when the patient's activity intolerances are reduced and his or her FR is expanded so that it encompasses home, sport, and work demands.
The Art, Science and Craft of the Clinical Method
- Evaluation - Hypothesis - Rx - Audit
- ID your patient's FR (history & exam)
- Rx treatments that are safe for your patients condition and have empirically been found to increase the FR.
- Always retest the FR posttreatment.
References
- Agency for Health Care Policy and Research (AHCPR). Acute Low-back Problems in Adults. Clinical Practice Guideline Number 14. Washington DC: U.S. Government Printing 1994.
- Cholewicki J, Simons APD, Radebold A. Effects of external loads on lumbar spine stability. Journal of Biomechanics 2000;33:1377-1385.
- Manniche C, et al. Low back pain: frequency management and prevention from an HAD perspective. Danish Health Technology Assessment (DIHTA), 1999.
- Jull GA. Deep cervical flexor muscle dysfunction in whiplash. Journal of Musculoskeletal Pain 2000;8:143-154.
- Kibler WB, Herring SA, Press JM. Functional Rehabilitation of Sports and Musculoskeletal Injuries. Aspen, 1998.
- Mannion AF, Junge A, Taimela S, Muntener M, Lorenzo K, Dvorak J. Active therapy for chronic low back pain, part 3: Factors influencing self-rated disability and its change following therapy. Spine 2001;26:920-929.
- McGill SM, Low back stability: from formal description to issues for performance and rehabilitation. Exerc Sport Sci Rev 2001;29(1):26-31.
- McGill SM. Spine instability. In: Liebenson C (ed) Rehabilitation of the Spine: A Practitioner's Manual, 2nd edition. Lippincott/Williams and Wilkins, Baltimore, 2003 (sched pub).
- McKenzie RA. Mechanical diagnosis and therapy for low back pain. In: Twomey LT, Taylor JR, eds. Physical Therapy of Low Back Pain. Churchill Livingstone, 1987.
- Morgan D. Concepts in functional training and postural stabilization for the low-back-injured. Top Acute Care Trauma Rehabil 1988;2(4):8-17.
- Radebold A, Cholewicki J, Panjabi MM, Patel TC. Muscle response pattern to sudden trunk loading in healthy individuals and in patients with chronic low back pain. Spine 2000;25:947-954.
- Radebold A, Cholewicki J, Polzhofer BA, Greene HS. Impaired postural control of the lumbar spine is associated with delayed muscle response times in patients with chronic idiopathic low back pain. Spine 2001;26:724-730.
- Richardson C, Jull G, Hides J, Hodges P. Therapeutic Exercise for Spinal Stabilization in Lower Back Pain. Churchill Livingstone, 2000.
- Vollowitz E. Furniture prescription for the conservative management of low-back pain. Top Acute Care Trauma Rehabil 1988;2(4):18-37.
Craig Liebenson,DC
Los Angeles, California
cldc@flash.net



